Key Takeaways
Summary: Dartmouth researchers published results from the FIRST-EVER randomized control trial on the effectiveness of an AI therapy chatbot in treating complex common mental health problems ranging from depression and anxiety, to eating disorders.
- Therabot, a generative AI chatbot, significantly reduced clinical symptoms of depression, anxiety, and eating disorders in just 4 weeks.
- Participants formed strong emotional bonds with the chatbot, rating it on par with human therapists in therapeutic alliance.
- Immediate, on-demand access may be the key to faster improvements that outpaces the effectiveness of traditional weekly therapy.
- The results challenge the traditional model of therapy and suggest a future where AI support isn’t optional—it’s essential.
- Therapists must evolve with this shift or risk being replaced by tools that can deliver scalable, personalized, and evidence-based care at any hour.
Why should you care? AI therapists like Therabot isn’t just reshaping therapy, it’s rewriting who gets help and how fast. This is a start wake-up call for Therapists: ADAPT OR DIE. These AI driven therapists could soon snatch their jobs through delivering faster, more effective, and scalable care that patients trust. We need to adapt to this tech or risk fading into obsolescence as the mental health world shifts beneath our feet.
Introduction
No glitzy headlines. No Silicon Valley fanfare. Just 106 people across the United States who is battling depression, anxiety, or eating disorders whos texting into a smartphone app late at night, early in the morning, on their lunch breaks. They weren’t talking to friends, or family. They were talking to Therabot, an AI therapist developed by researchers from Dartmouth University.
And here’s the shocker: it worked. REALLY WELL.
In fact, this AI Therapist helped these people reduce their depression symptoms by 51%, anxiety by 31%, and even showed significant results in treating eating disorders (an area where traditional therapeutic approaches often struggles with). And these weren’t just mild or almost clinically non-significant improvements either. Thessaasda were large, significant and sustainable changes that would normally take months of intensive human-led therapy. And guess what? It happened in just four weeks of use… with zero pills, zero waitlists and zero time limits!.. just real-time interventions when it was needed most. Just type and talk.

These results was part of the first randomized controlled trial to prove what some therapists have long feared and what many patients have quietly hoped: a generative AI chatbot, trained on evidence-based therapy techniques, can not only match the results of human therapists but it can outperform them and in a much shorter time.
That’s not hype. That’s data.
A Chatbot That Feels Like a Therapist
Dartmouth researchers built the smartphone based Therabot, an AI chatbot which was was trained on thousands of hours of evidence-based cognitive behavioral therapy (CBT) discussions between therapists and clients in order to deliver real effective CBT to participants in real time. Over eight weeks, 106 people who were diagnosed with depression, anxiety, or eating disorders were able to use the app (in which ever way they saw fit). They didnt need to make appointments, there was no waiting rooms and no time limits to the conversations.
By week four, the participants saw drastic changes in their self-reported mental health problems symptoms. As mentioned before, they saw a massive reduction in depression (51% lower then baseline), anxiety (31% reduction) and even concerns about body image and weight were reduced by 19%… All out performing the treat outperforming the waitlist control group.
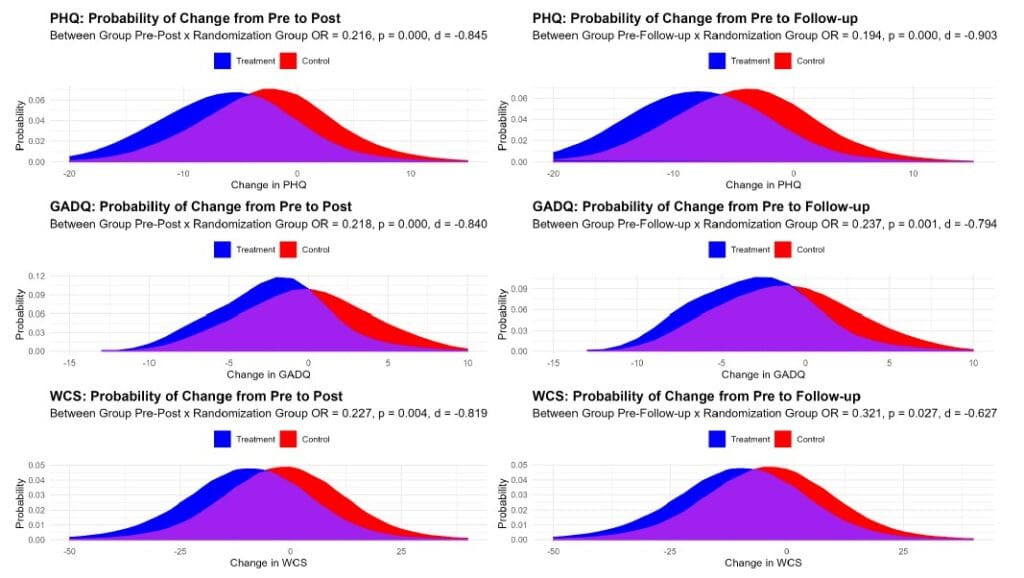
weight/shape concerns, row-wise) at post (4 weeks, left column) and follow up (8 weeks, right column). Treatment group is visualized in blue and control in red (Heinz et al. , 2025)
But thats not the most interesting part… the most surprising finding of the study was….
Participants said they felt connected to Therabot. They trusted it. They initiated conversations with it, not because they were prompted, but because they wanted to.
For example, one participant in the study initiated over 1,500 messages in just eight weeks. Another logged on consistently at 2 a.m. when they experienced their panic attacks to be at their worst and when therapists are obviously asleep. What they found wasn’t a sterile machine spewing jargon. It was something else. Therabot asked, “Why do you think you feel that way?” It validated. It remembered. It adapted. And most remarkably… it was empathic, it understood and it didn’t judge.
This, perhaps, is the real secret behind its success. Unlike traditional digital health apps that often feel transactional, Therabot created something precious: a true therapeutic alliance. The same kind of bond patients report with human therapists. The kind of trust that makes healing possible.
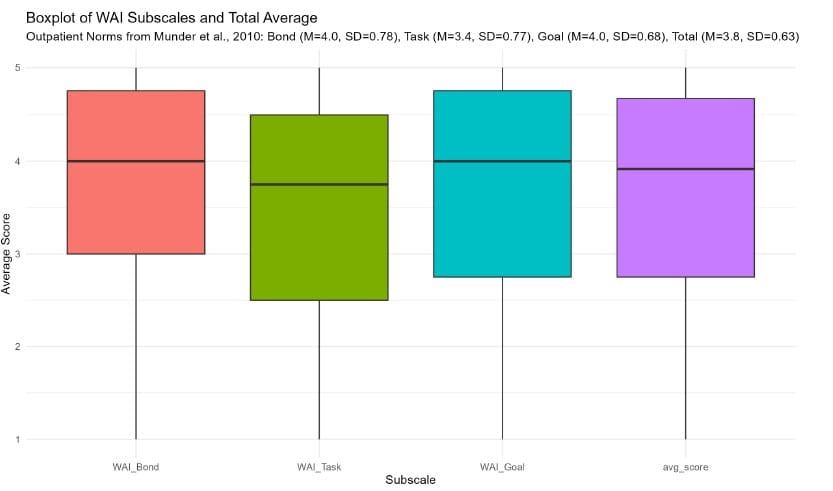
The paper showed this by also assessing the clinical alliance between the participants and Therabot (which is the same ones clinicians use to assess the relationship/bond with a patient). Their results showed that Therabot scored just as high as a real therapist.
The Myth of the 50-Minute Hour
We’ve long accepted the model of therapy as a weekly appointment. Fifty minutes, once a week. You talk. Your therapist listens. Then you wait seven days to do it again. But the human mind doesn’t schedule its pain so neatly.
Therabot was always on. Participants used it when they needed to, for as long as they needed to. And that’s what made the difference.
What the Therabot trial revealed is something therapists already know, but most systems can’t accommodate: people don’t suffer in 50-minute blocks. Anxiety hits at midnight. Depression creeps in after a bad meeting. Body image spirals don’t wait for Thursday at 3:00 p.m.
That real-time, just-in-time access may be the secret to why it worked so well, so quickly.
It’s not that AI is better than humans at therapy. It’s that humans are trapped inside a model that can’t flex with real life. The chatbot isn’t better… its as effective and its it’s just there when needed.
But Is It Safe?
Let’s be honest. The idea of a machine providing mental health care feels unsettling to many. What if it gets something wrong? What if it “hallucinates” a harmful suggestion?
The researchers anticipated this and built in a number of fail-safes. Therabot wasn’t just left to roam the wild. It was equipped with crisis detection systems, instant emergency protocols, and was fine-tuned with thousands of therapist-reviewed scripts. In total, over 100,000 hours of human labor shaped its brain.
And critically… every word it said during the trial was monitored for safety.
This wasn’t an experiment in replacing humans. It was an exploration of what happens when humans and machines work together.
Should This Make Therapists Nervous?
Let’s be honest. Most digital mental health tools have been underwhelming. Wellness apps. Guided journaling. Chatbots that sound like a customer service agent in disguise.
But this is different. Therabot wasn’t trained to talk about the weather. It was trained to treat clinical disorders—backed by evidence, supervised by psychiatrists, and tested with scientific rigor.
And now it has something no other app has: peer-reviewed proof that it can deliver real therapeutic results at scale.
That’s why therapists.. well… the entire mental health profession… should be paying very close attention.
Not because they’re obsolete. But because they’re unprepared.
If a machine can deliver the equivalent of eight therapy sessions over text, and help people feel better, faster, and at any time of day…. then what exactly is the role of a therapist who only sees patients once a week? It’s a hard question. But it’s also an opportunity.
I think therapists who embrace this shift who learn how to work with AI and use it between sessions as a means to provide additional support and provide personalize interventions will not only extend their reach, but help improve the effectiveness of their care. And those who don’t… well… they may be replaced by something that never sleeps.
And now the kicker… We’re Already Behind
Keep in mind: the Therabot trial concluded in June 2024, way before ChatGPT 4.5, before emotion recognition APIs, before multimodal models, before MCP, before AI could analyze tone of voice and facial expression in real time….
So that was then.
If a basic text-based chatbot could deliver this much therapeutic value last year, just imagine what today’s models can do.
The idea that “AI will never replace human therapists” sounds noble. But maybe it’s naive. It assumes people prefer humanity to accessibility, nuance to immediacy. But when you’re spiraling at 1 a.m., and something that feels like it understands you is only a tap away?
You don’t need perfection. You need relief.
So Where Do We Go From Here?
We’re not suggesting a wholesale replacement of therapists. Humans will always matter and especially for complex trauma, crises, and long-term growth. But we are saying this: therapy is no longer just a human business. It’s a hybrid one.
The professionals who thrive in the next decade won’t be the ones defending the old ways. They’ll be the ones who adapt, who integrate, who see AI not as a threat, but as an extension of care. Because whether we like it or not, the chatbot will see you now.
And for millions of people who’ve been waiting for help, that might be the best news they’ve heard in a long time.
References
Heinz, M. V., Mackin, D. M., Trudeau, B. M., Bhattacharya, S., Wang, Y., Banta, H. A., … & Jacobson, N. C. (2025). Randomized Trial of a Generative AI Chatbot for Mental Health Treatment. NEJM AI, 2(4), AIoa2400802.





